
Minimally invasive spine surgery (MISS) in Pune is performed by Dr. Sarang Gotecha at Manipal Hospital, Baner - fellowship-trained in Seoul, South Korea. MISS treats lumbar disc herniation, spinal stenosis and single-level instability through incisions under 2 cm, with discharge typically within 24–48 hours and return to light work in 2–3 weeks.
Unique Most patients in Pune who need spine surgery do not know that MISS exists as an option - they assume 'spine surgery' means weeks in hospital, a large scar and months of recovery. Open with the contrast between what patients expect and what MISS can actually deliver. Use Dr. Gotecha's Seoul fellowship as proof that this isn't experimental - it is internationally established and he brought it to his Pune practice.
There is a significant gap between what most people believe spine surgery involves and what modern minimally invasive techniques can actually deliver. Most patients arrive for a consultation expecting to be told they need a large incision, 7–10 days in hospital and 3–4 months before they can work again. For many of them, that picture is outdated.
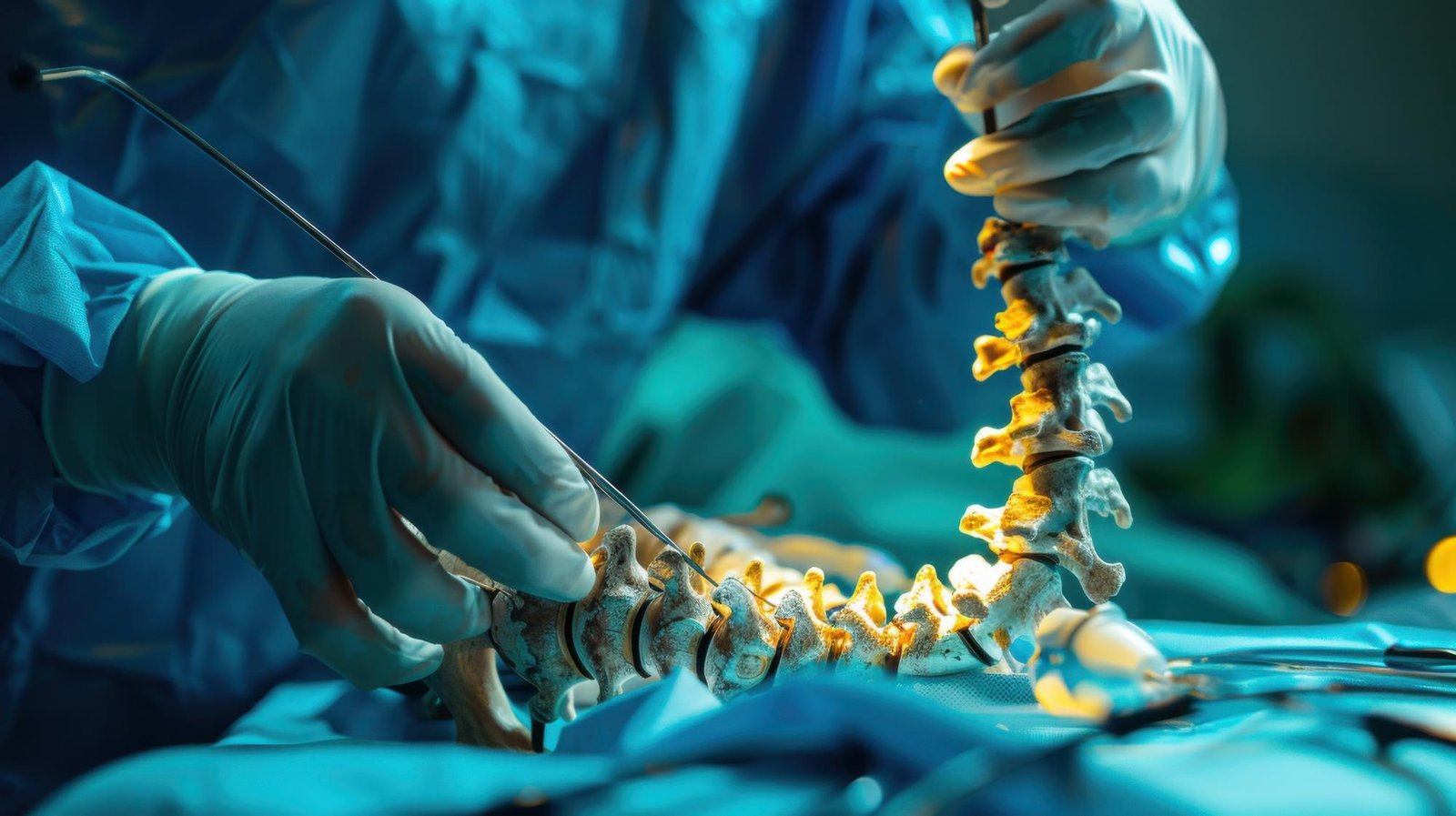
Minimally invasive spine surgery (MISS) uses tubular retractors, endoscopes and percutaneous (through-the-skin) instruments to achieve the same surgical goals as open surgery - decompression, stabilisation, fusion - through incisions as small as 1–2 cm. The muscles alongside the spine are dilated rather than cut, preserving the muscle bulk that is critical for long-term back strength and stability.
Dr. Sarang Gotecha completed a dedicated Fellowship in Minimally Invasive Spine Surgery at St. Mary's Hospital, Catholic University of Korea, Seoul - one of Asia's leading centres for MISS training. He brought this expertise back to his Pune practice at Manipal Hospital, Baner.
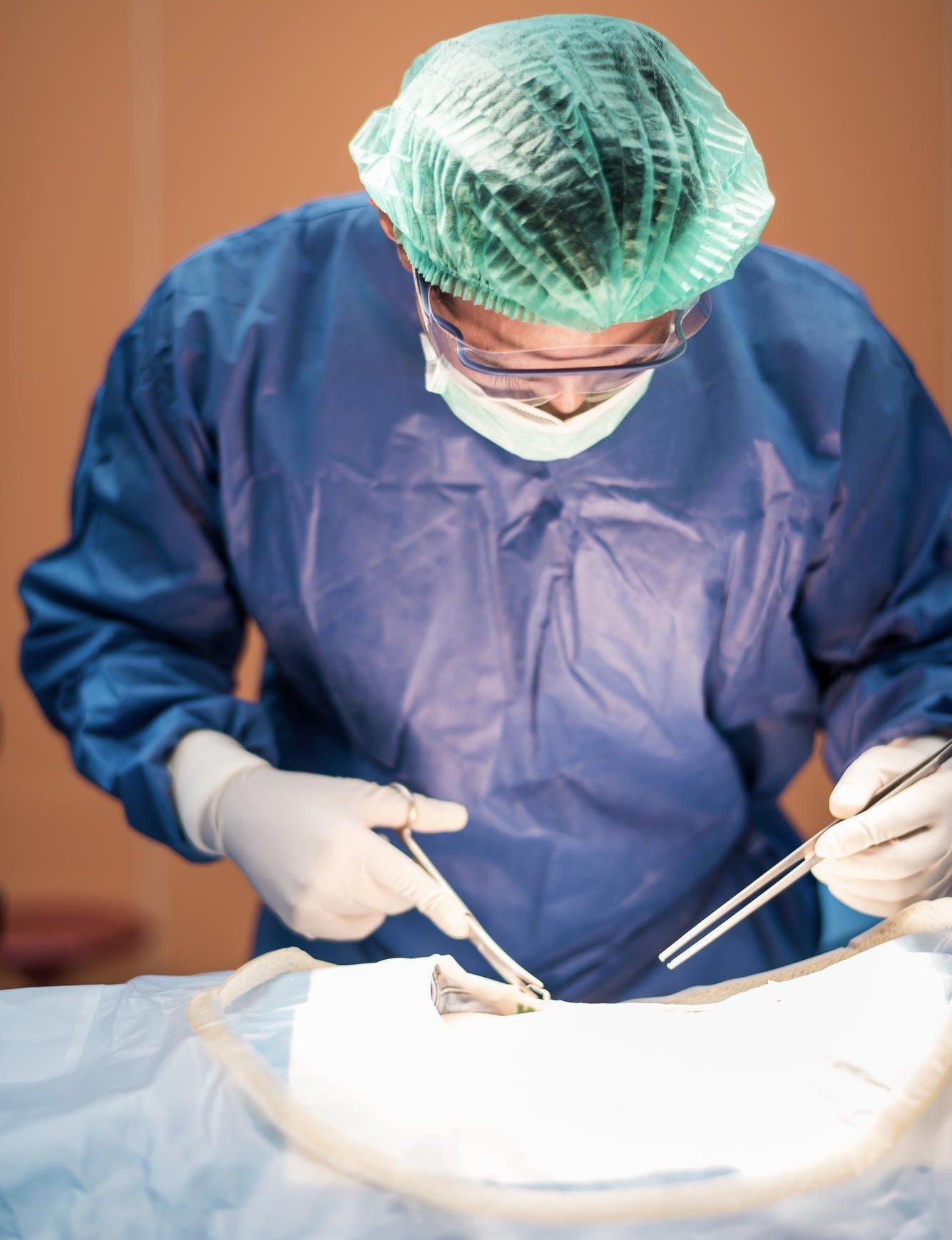
In traditional open spine surgery: A long incision is made along the spine. The muscles on either side are cut and retracted (pulled aside) to expose the bone and disc. This muscle damage is a significant source of post-operative pain and prolonged recovery.
In minimally invasive spine surgery: A small skin incision (1–2 cm) is made. A series of dilating tubes, each slightly larger than the last, are inserted to create a working channel through the muscle - parting rather than cutting the fibres. A tubular retractor holds this channel open while the surgeon works through a microscope or endoscope.
The result: equivalent decompression or fusion with dramatically less soft-tissue trauma, less blood loss, less post-operative pain and significantly shorter recovery.
This is the most common indication for MISS. When a lumbar disc herniates and compresses a nerve root, causing sciatica (leg pain, numbness, weakness), a microdiscectomy via a tubular retractor removes the prolapsed disc fragment and relieves nerve pressure. The procedure takes 45–60 minutes and most patients walk the same day.
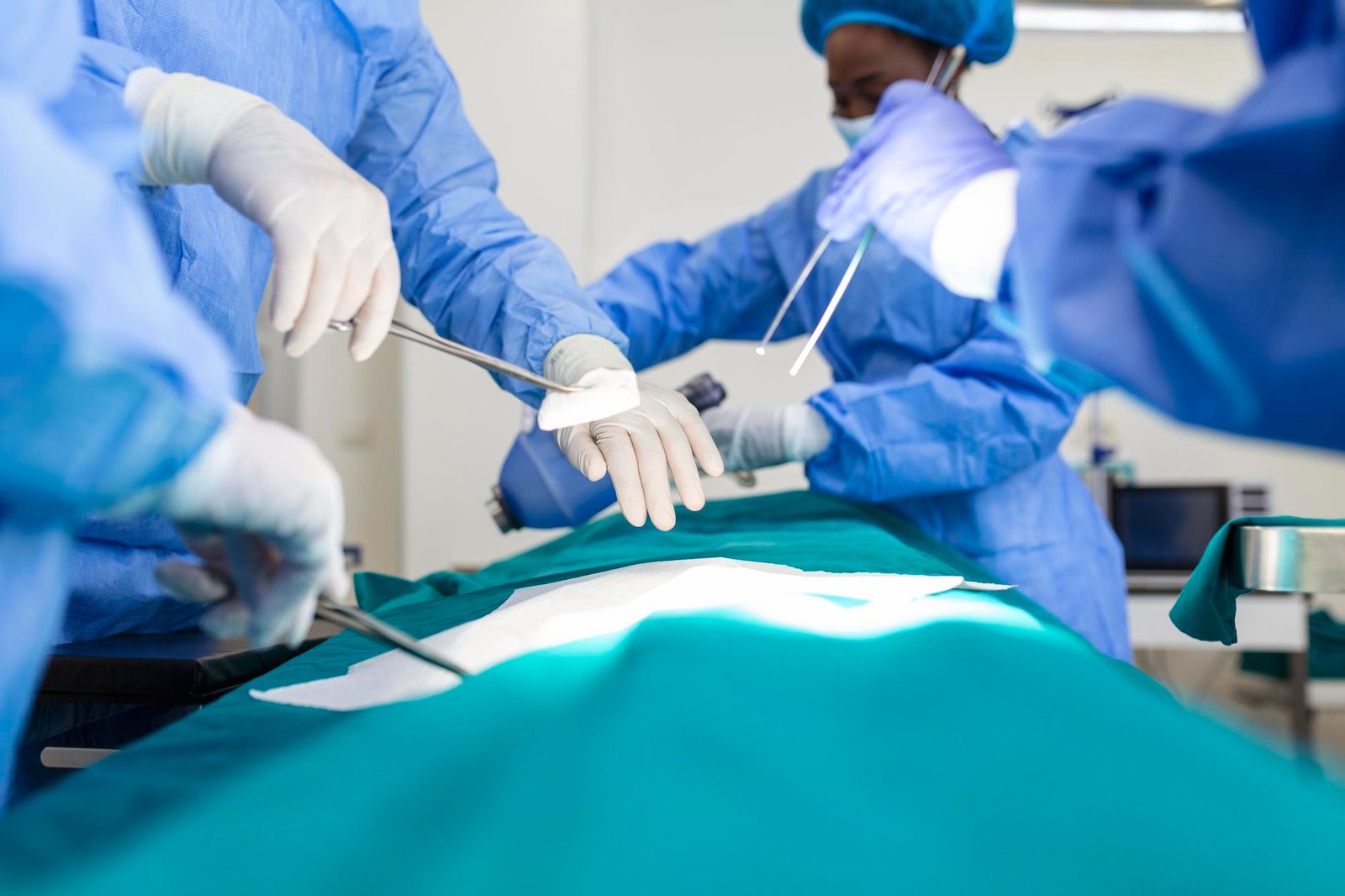
Narrowing of the spinal canal (stenosis) due to degenerative changes - thickened ligaments, bone spurs - causes leg pain on walking (neurogenic claudication). Endoscopic or tubular laminotomy decompresses the canal through a single small incision, avoiding the need for fusion in many cases.
Minimally Invasive Transforaminal Lumbar Interbody Fusion (MIS-TLIF) addresses spinal instability (spondylolisthesis, degenerative disc disease with segmental instability) through two small paramedian incisions. Percutaneous pedicle screws provide fixation without exposing or damaging the posterior spinal muscles.
A 16–18 mm tubular retractor is placed over the affected disc level. Under operating microscope magnification, the herniated disc fragment is removed with minimal disruption to adjacent structures. This is the workhorse MISS procedure for lumbar disc herniation.
Pedicle screws are inserted through small stab incisions using fluoroscopic (X-ray) guidance, avoiding the large muscle-stripping exposure required for open screw placement. Rods connecting the screws are passed beneath the skin. This technique is used for fusion procedures and spinal fracture fixation.
The most advanced form of MISS - a 7–8 mm endoscope with an integrated working channel is inserted either through the skin at the side of the spine (transforaminal approach) or through the back (interlaminar approach). The entire procedure is performed through this single instrument, watching on a monitor. It requires the highest level of surgical skill and is not widely available in Pune outside specialist centres.
• Patients with single or two-level disc herniation or stenosis without significant deformity
• Those requiring single-level fusion for instability or spondylolisthesis
• Patients who are medically fit for anaesthesia
• Those who want faster recovery - particularly working-age adults who need to return to employment
MISS may not be the best approach for: multi-level complex deformities, severe osteoporosis, or revision cases with significant scar tissue from prior surgery. Dr. Gotecha evaluates candidacy based on MRI, CT and clinical findings at consultation.
• Blood loss: MISS - 50–100 mL; Open - 200–500 mL for comparable procedures
• Hospital stay: MISS - 1–2 days; Open - 4–6 days
• Post-operative pain: MISS - significantly less (less muscle damage)
• Return to work: MISS - 2–3 weeks (desk job); Open - 6–8 weeks
• Suitability: Open surgery remains better for complex, multi-level, or revision cases
• Surgical time: MISS often takes slightly longer; the technical precision required is higher
Dr. Gotecha does not recommend MISS because it is technologically impressive. He recommends it when it is the right choice for a specific patient's anatomy, condition and life circumstances.
