
Neuroendoscopic surgery in Pune, performed by Dr. Sarang Gotecha at Manipal Hospital, Baner, uses a thin endoscope through a small burr hole to treat hydrocephalus, arachnoid cysts, colloid cysts and intraventricular tumors. It avoids large incisions, reduces recovery time and is particularly effective for hydrocephalus via endoscopic third ventriculostomy (ETV).
Neuroendoscopy is widely available in the US and Europe but remains underutilised in most Indian cities outside tier-1 metros. Lead with the fact that many patients who receive a VP shunt (the traditional treatment for hydrocephalus) could instead be candidates for ETV - a one-time procedure with no implant, no shunt and no risk of shunt malfunction. Dr. Gotecha's training makes this option available in Pune when it is clinically appropriate.
The brain is enclosed in a rigid skull. Any surgical access to it demands respect for anatomy and a strong rationale for why the risk of opening the skull is justified by the benefit of the procedure. Neuroendoscopy is a technique that shifts this calculus significantly in the patient's favour.
Instead of a large craniotomy (removing a section of the skull), neuroendoscopy accesses the brain through a small burr hole - typically 1–1.5 cm - through which a thin, lighted endoscope with a camera is inserted. The surgeon operates by watching a high-definition monitor, using instruments passed alongside the endoscope. The result is surgical access to deep brain structures that previously required large, complex open approaches.
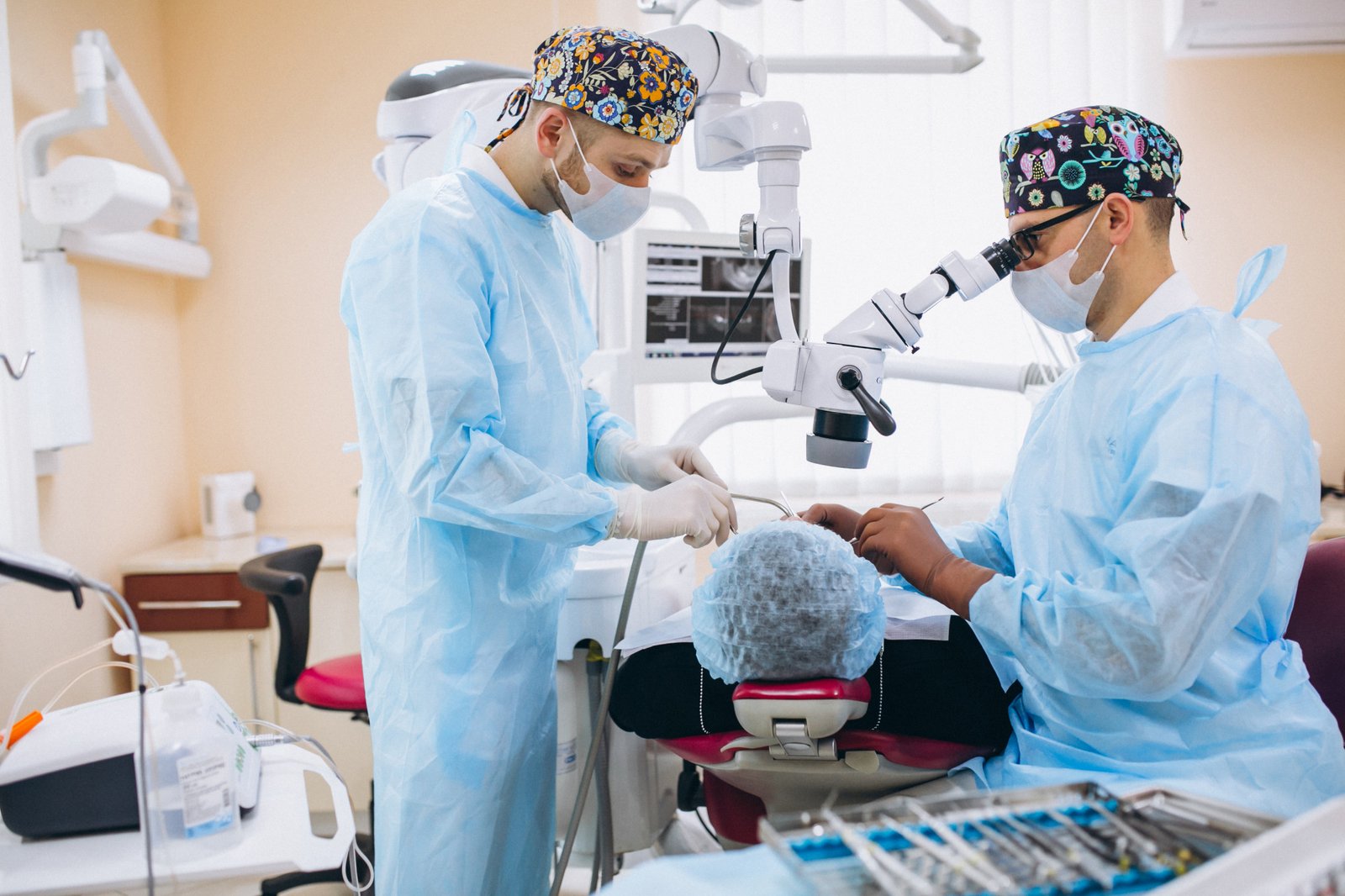
Dr. Sarang Gotecha, MCh Neurosurgery, performs neuroendoscopic surgeries at Manipal Hospital, Baner, Pune. He sees patients at clinics in Wakad and Thergaon for pre-operative consultation and post-operative follow-up.
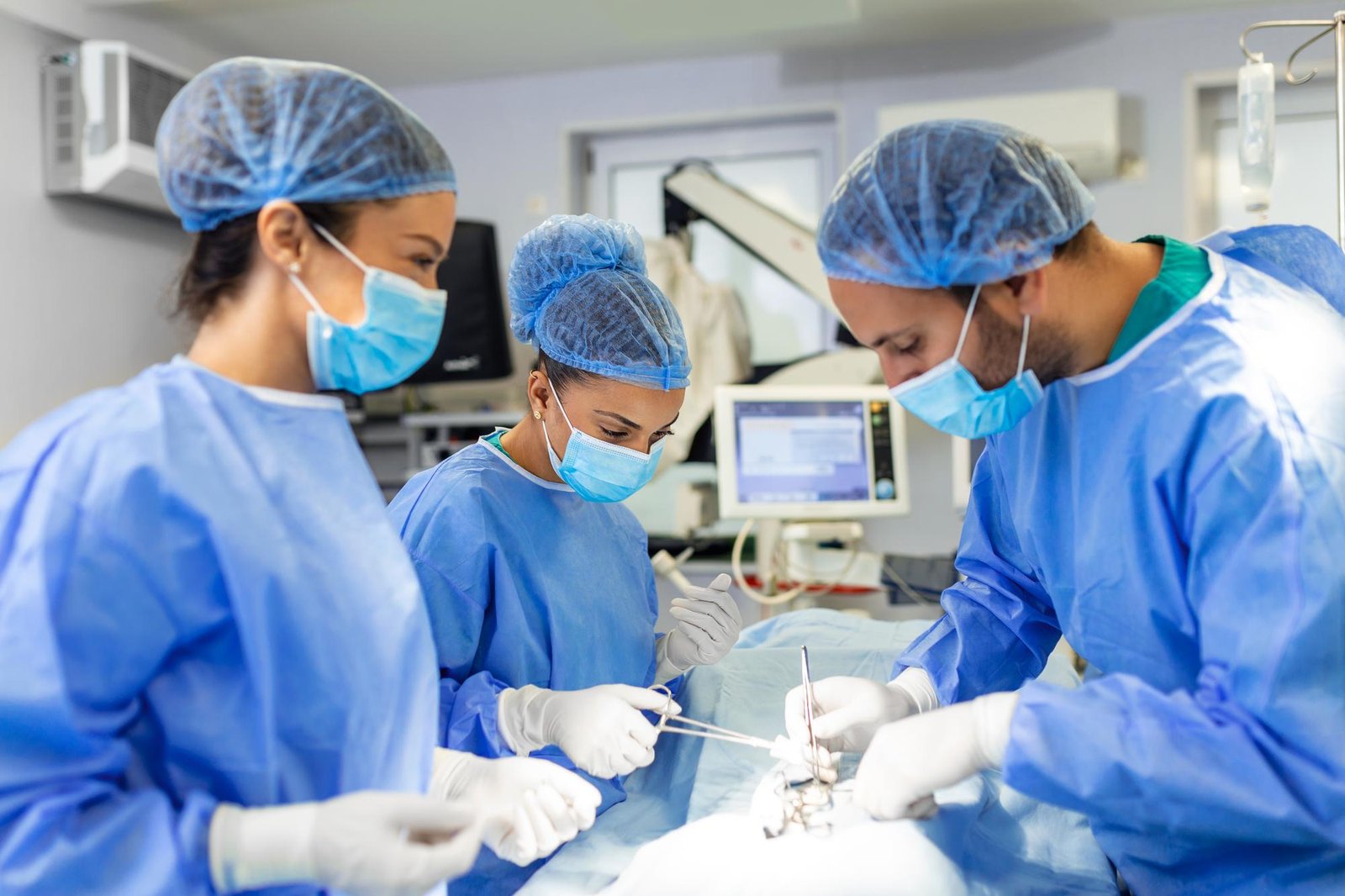
Neuroendoscopy uses a rigid or flexible endoscope inserted through a small burr hole in the skull. The endoscope carries fibre-optic light and a camera, transmitting real-time images to a high-resolution monitor. Surgical instruments - scissors, graspers, coagulation probes - are passed through working channels in the endoscope.
The approach avoids the need for large incisions and brain retraction (physically moving the brain aside to access deep structures), which is a significant source of neurological injury in older surgical techniques. Patients who undergo neuroendoscopic procedures typically experience:
• Shorter anaesthesia duration
• Less intraoperative blood loss
• Shorter ICU stay
• Faster return to daily activities
Hydrocephalus is an abnormal accumulation of cerebrospinal fluid (CSF) in the brain's ventricular system, causing increased pressure within the skull. It can occur in children (often due to congenital causes or meningitis) and adults (due to tumors, haemorrhage, or aqueductal stenosis).
Traditionally, hydrocephalus was treated with a VP shunt - a tube that drains CSF from the brain ventricle to the abdominal cavity. Shunts work well but carry long-term risks: shunt blockage, infection, over-drainage and the need for revision surgery over a patient's lifetime.
ETV is an endoscopic procedure that creates a small opening in the floor of the third ventricle, allowing CSF to bypass the obstruction and flow naturally. In suitable candidates - those with obstructive hydrocephalus - ETV has a success rate of 60–80% and, when successful, eliminates the need for a shunt entirely. Dr. Gotecha carefully selects candidates for ETV using clinical criteria and MRI analysis.
Colloid cysts are benign cysts that form in the third ventricle of the brain . Despite being non-cancerous, they can block CSF flow and cause sudden increases in intracranial pressure - in rare cases, this can be fatal. Endoscopic removal of colloid cysts is the preferred approach, accessing the cyst through the foramen of Monro via a burr hole and removing it under direct vision.
Arachnoid cysts are fluid-filled sacs that form within the brain's coverings (arachnoid membrane). Many are asymptomatic and require only monitoring. When they cause headaches, seizures, or focal neurological symptoms, endoscopic fenestration - creating an opening between the cyst and the normal CSF spaces - relieves pressure without large incisions.
Some tumors grow within the brain's ventricles - ependymomas, subependymomas, choroid plexus papillomas. Neuroendoscopy allows biopsy (tissue sampling) and, in selected cases, partial or complete removal of these tumors through a minimal-access approach.
This is one of the most common questions families ask when a loved one is diagnosed with hydrocephalus. There is no universal answer, but the thinking has evolved significantly.
ETV is preferred when: The hydrocephalus is obstructive (not communicating), the patient is older than 6 months (success rates are lower in very young infants) and MRI shows a suitable anatomy for third ventriculostomy. VP Shunt is preferred when: ETV has failed, the hydrocephalus is communicating (CSF absorption is impaired rather than flow being blocked), or the patient's anatomy is not suitable for ETV.In practice, Dr. Gotecha reviews each patient's imaging and clinical picture carefully before recommending one over the other. Both are valid treatments - the goal is to choose the one most likely to work durably for that specific patient.
The procedure is performed under general anaesthesia. A small burr hole is made in the skull (typically at the hairline, so any scar is hidden). The endoscope is inserted and the procedure completed - ETV typically takes 30–60 minutes. The patient wakes in recovery and is monitored in a high-dependency or ICU setting overnight.
Most patients are discharged within 2–4 days. Follow-up MRI is scheduled at 3 months to assess the outcome (for ETV, to confirm CSF flow through the ventriculostomy). Headaches and mild fatigue in the first week are normal.
For patients coming from Wakad, Thergaon, or Chinchwad - the short distance to Manipal Hospital, Baner , makes follow-up appointments significantly easier than travelling to Pune's more central hospitals.
