
Cerebrovascular surgery in Pune, performed by Dr. Sarang Gotecha at Manipal Hospital, Baner, addresses brain aneurysms, arteriovenous malformations (AVMs) and cavernomas using microsurgical clipping and AVM resection. His training at the National Neuroscience Institute, Singapore, included extensive cerebrovascular case exposure, making him one of Pune's experienced vascular neurosurgeons.
Open with an alarming but actionable fact: Brain aneurysms affect approximately 2–5% of the general population and up to 10–15% of people who suffer a rupture die before reaching hospital. The survivors who reach a neurosurgical centre have roughly a 30-day mortality risk of 40–50% without surgical intervention. In Pune, access to a surgeon trained in microsurgical clipping at a fully equipped centre is not a luxury - it is the difference between survival and death. Frame this not to frighten but to explain why knowing your options before a crisis matters.
Conditions affecting the blood vessels of the brain sit in a different category from most neurosurgical problems. With a brain tumor or a herniated disc, time typically allows for careful consultation, second opinions and planned surgery. With a ruptured brain aneurysm, hours - sometimes minutes - determine whether a patient survives neurologically intact or does not survive at all.
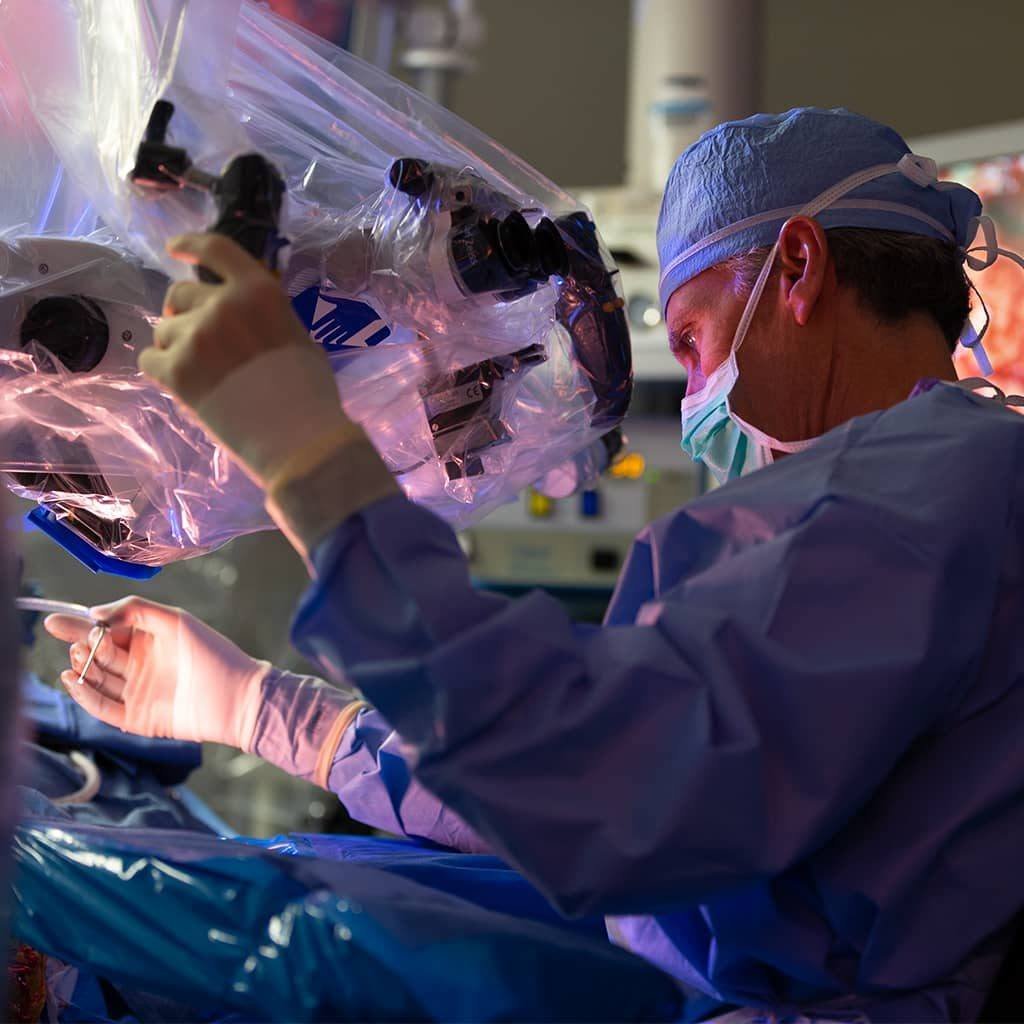
Cerebrovascular surgery encompasses the surgical management of all vascular abnormalities within the brain and its covering structures - aneurysms, arteriovenous malformations, cavernomas and related conditions. Dr. Sarang Gotecha has received training in these complex procedures, including significant exposure during his WFNS Fellowship at the National Neuroscience Institute, Singapore and his observership at Tan Tock Seng Hospital.
He performs cerebrovascular surgery at Manipal Hospital, Baner - the facility in western Pune best equipped to handle vascular neurosurgical emergencies with appropriate anaesthesia, neuro-ICU and intraoperative monitoring support.
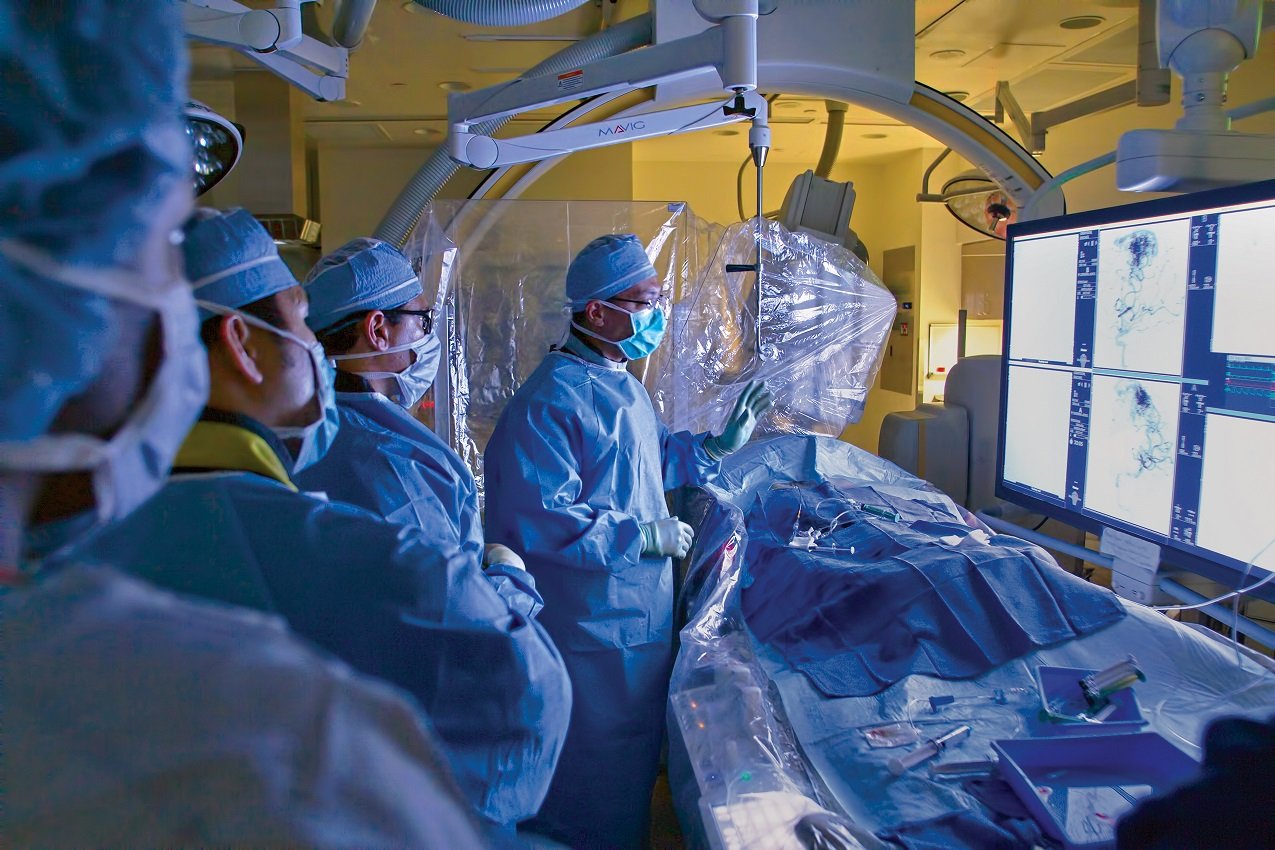
Cerebrovascular surgery involves operating on the blood vessels of the brain - arteries and veins - to correct structural abnormalities that cause symptoms or pose life-threatening risks. Unlike interventional neuroradiology (which treats some of these conditions via catheters through blood vessels), microsurgical cerebrovascular surgery directly accesses the lesion through a craniotomy.
Both approaches - open microsurgery and endovascular intervention - have their place. The choice depends on the lesion's anatomy, location, size and the patient's overall clinical status. Dr. Gotecha discusses both options where both are applicable.
A brain aneurysm is a balloon-like bulge in the wall of a brain artery, caused by a weak spot in the vessel wall. Most aneurysms cause no symptoms until they rupture, releasing blood into the subarachnoid space (subarachnoid haemorrhage - SAH). Rupture is typically heralded by the 'worst headache of my life' - a sudden, severe, thunderclap headache.
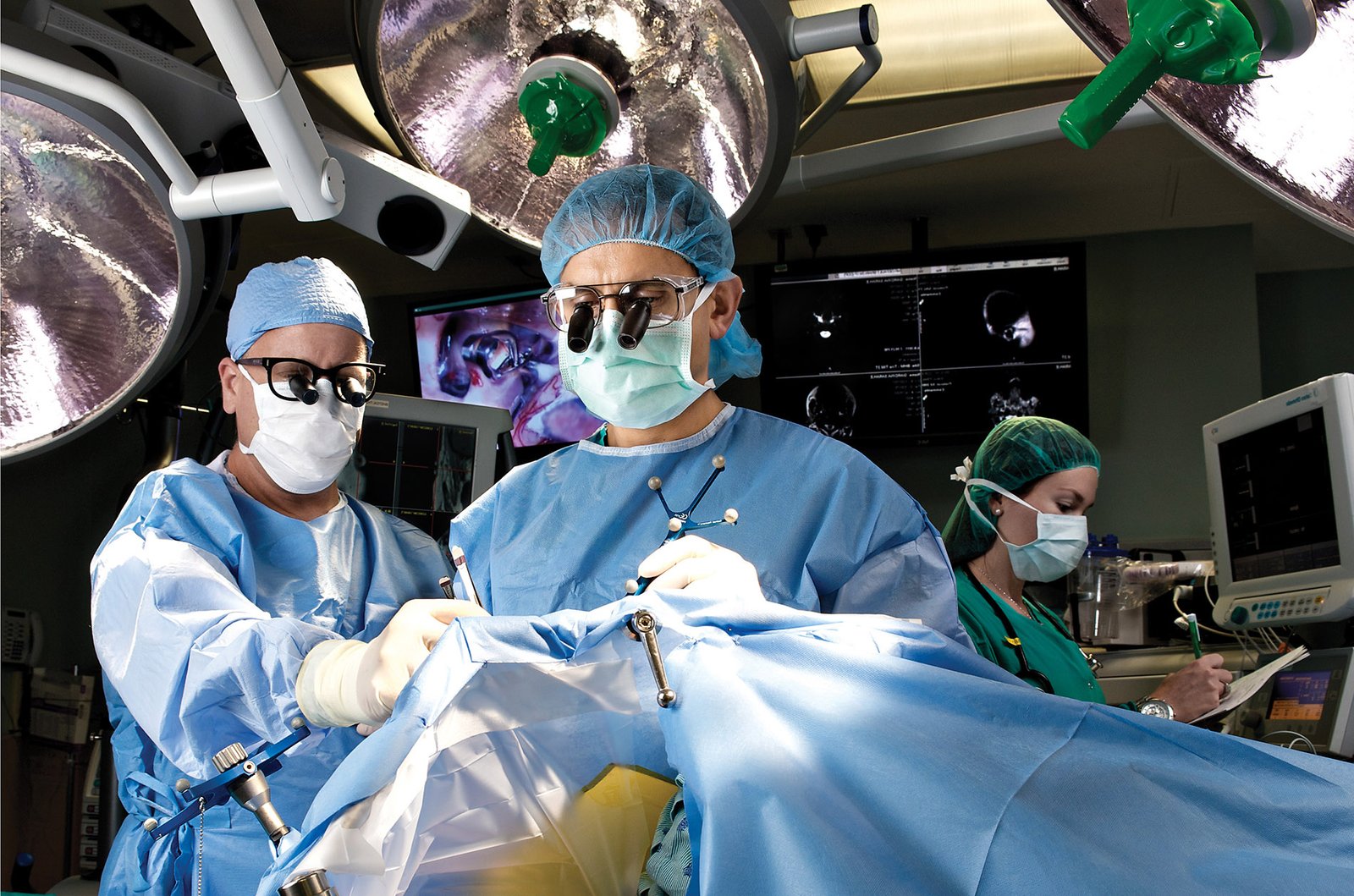
Unruptured aneurysms found incidentally during imaging for other reasons require careful risk assessment: the annual rupture risk, the patient's age and health and the surgical risk of clipping must all be weighed. Small aneurysms in older patients with significant medical comorbidities may be observed. Larger aneurysms, those with specific shapes or locations, or those in younger patients are generally treated.
Surgical clipping involves placing a small metal clip across the aneurysm's neck, cutting off its blood supply while preserving the parent artery. When technically feasible, clipping provides definitive cure - the aneurysm is eliminated and the risk of re-rupture goes to near zero.
An AVM is an abnormal tangle of blood vessels connecting arteries and veins in the brain, bypassing the normal capillary network. Blood flows under arterial pressure directly into veins, which are not built to handle it. AVMs can bleed (intracerebral haemorrhage), cause seizures, or produce progressive neurological deficits due to blood 'stealing' from adjacent normal brain.
Treatment options include microsurgical resection, stereotactic radiosurgery (Gamma Knife), or endovascular embolisation - often used in combination. For small, superficial AVMs in non-eloquent brain areas, surgical resection provides the best single-procedure cure rate. Dr. Gotecha assesses AVM cases using the Spetzler-Martin grading system, which guides treatment selection.
Cavernomas are clusters of abnormally dilated small blood vessels (cavernous sinusoids) within the brain. They bleed repeatedly in small amounts - not catastrophically like aneurysms, but enough to cause cumulative neurological symptoms: headaches, seizures, focal deficits. When a cavernoma has bled once (especially in an accessible location), surgical removal carries a much lower long-term risk than waiting for re-bleeding.
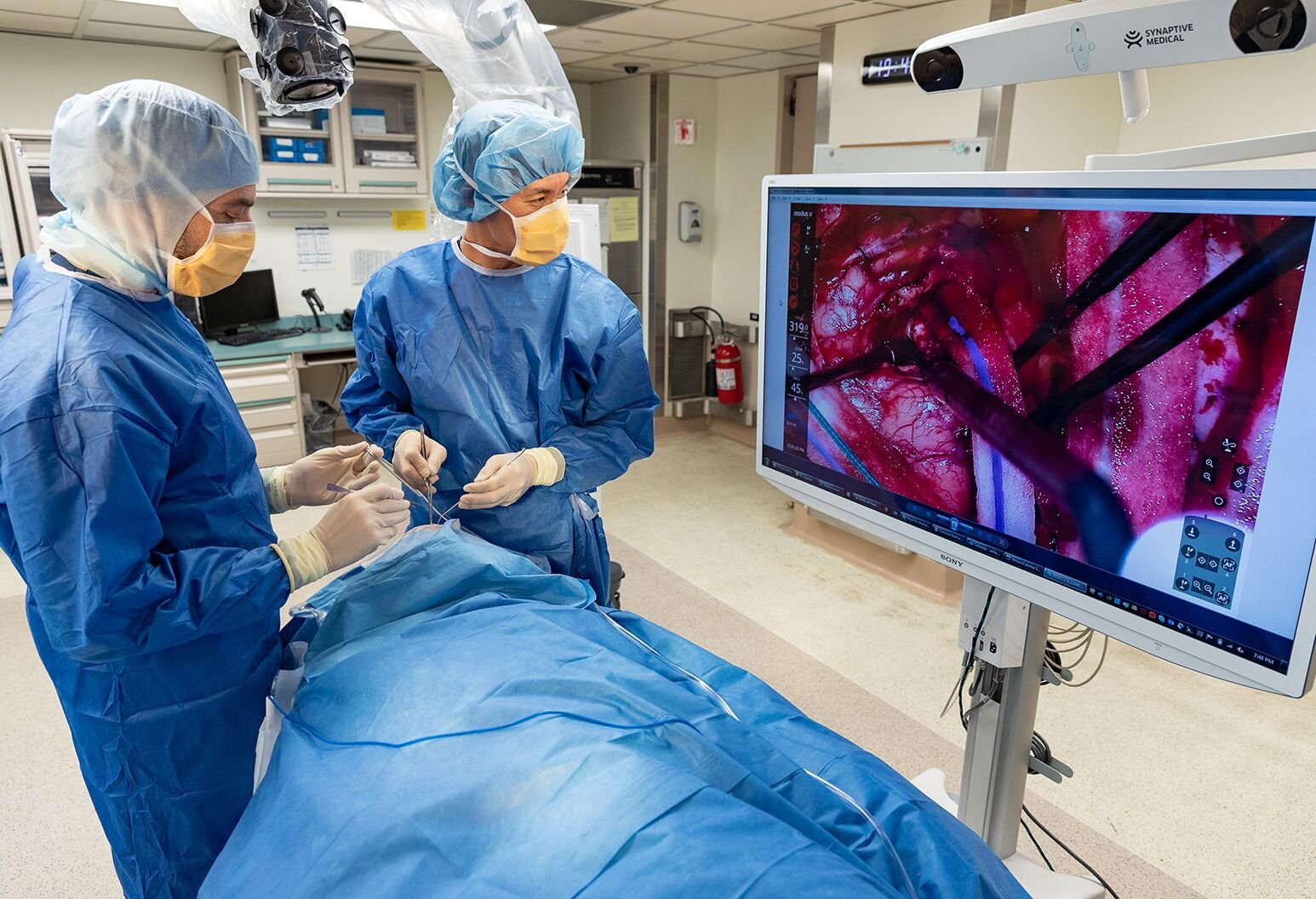
The patient is positioned on the operating table with the head fixed in a three-point head holder. A craniotomy (carefully planned based on pre-operative imaging) exposes the relevant part of the brain and its arteries. The surgeon works under the operating microscope - typically at 10–15x magnification - carefully dissecting the brain's natural spaces (cisterns) to reach the aneurysm.
A titanium aneurysm clip is then applied across the aneurysm neck. Intraoperative blood flow is assessed (using Doppler or fluorescein angiography) to confirm the parent artery is patent and the aneurysm is excluded. The craniotomy is closed and the patient is monitored in the neuro-ICU.
For ruptured aneurysms, the goal is to secure the aneurysm as quickly as safely possible to prevent re-rupture, then manage the complications of subarachnoid haemorrhage - vasospasm, hydrocephalus - over the subsequent 2 weeks.
• Sudden, severe headache unlike any previous headache (rupture - seek emergency care immediately )
• Drooping eyelid with dilated pupil on one side (posterior communicating artery aneurysm compressing the oculomotor nerve)
• Double vision
• Pain above or behind the eye
Incidentally discovered aneurysms on MRI or CT done for another reason require neurosurgical consultation to assess rupture risk and management options.
Not every AVM requires surgery. Grade I-II AVMs (small, superficial, non-eloquent location on Spetzler-Martin scale) are excellent surgical candidates - the cure rate with resection is near 90% with acceptable surgical risk. Grade IV–V AVMs (large, deep, or in eloquent areas) carry prohibitive surgical risk and are often managed with radiosurgery or observation.
Dr. Gotecha discusses the Spetzler-Martin grade of each AVM with the patient, explaining what Grade I through V means practically - not just the number, but what it implies about surgical risk versus natural history risk.
